Occasional heartburn after a heavy meal is not uncommon. However, if you find yourself relying on antacids frequently or experiencing persistent chest discomfort or tightness, it may be a sign of gastroesophageal reflux disease (GERD).
GERD is more than simple indigestion. It is a chronic condition in which stomach acid repeatedly flows back into the oesophagus and may require proper assessment and management.
Understanding its causes and how it can be prevented is an important first step.
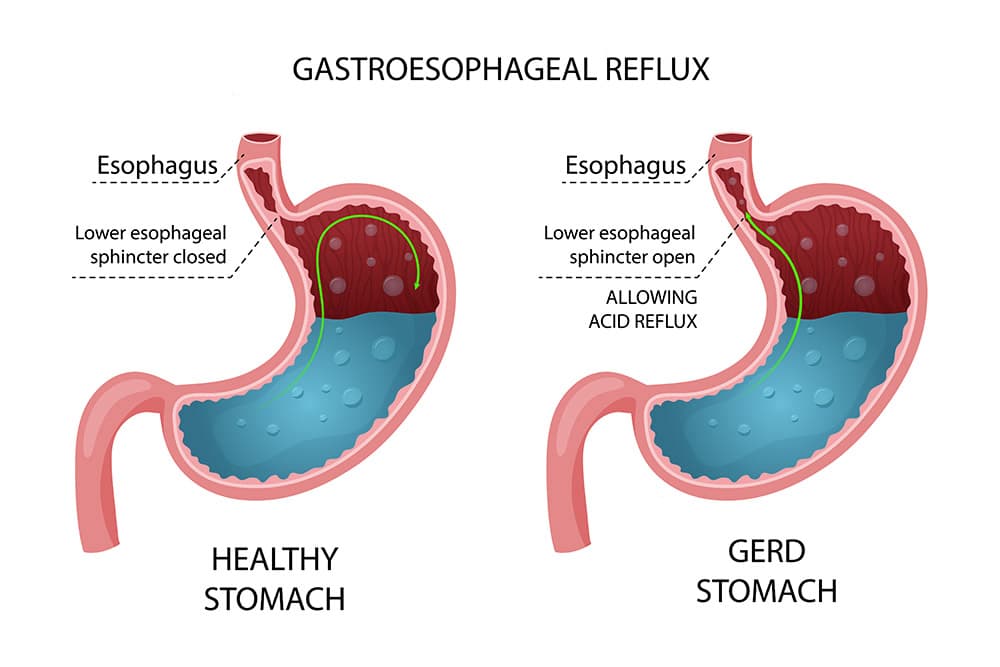
GERD: A closer look
GERD is often described as a burning sensation in the chest. It occurs when stomach acid repeatedly flows back into the oesophagus. This acid reflux irritates the lining of your oesophagus, causing symptoms such :
- A burning sensation in the chest (heartburn), especially after eating or when lying down
- Sour taste or sensation of fluid in the back of the throat
- Difficulty swallowing or feeling of food “stuck” in the chest
- Chronic cough, hoarseness or throat clearing
- Disrupted sleep from nighttime reflux
Occasional acid reflux can affect anyone. However, when symptoms occur more than twice a week or begin to interfere with daily activities, it is generally considered gastroesophageal reflux disease (GERD).
What causes GERD?
GERD is most commonly caused by weakness or dysfunction of the lower oesophageal sphincter (LES), the muscle valve between your stomach and oesophagus. When this valve relaxes abnormally or weakens, stomach acid can flow back into the oesophagus.
Common contributing factors and triggers of acid reflux or GERD include:
- Large or heavy meals, which increase pressure within the stomach
- Lying down or going to bed soon after eating
- Excess body weight or pregnancy, both of which increase abdominal pressure
- Hiatal hernia, where part of the stomach moves upward into the chest
- Certain foods and beverages, including caffeine, alcohol, chocolate, and spicy or fatty foods
- Smoking
- Certain medications, such as anti-inflammatory drugs or sedatives
In addition, some individuals may be at higher risk of developing GERD. These include pregnant women, frequent alcohol consumers, individuals who are overweight and those with a family history of reflux.
Young adults with high stress levels or irregular eating habits may also experience GERD symptoms.
Why GERD feels worse at night
Many people notice that reflux symptoms become more pronounced at night, particularly when lying down. This is not uncommon and has a physiological explanation.
When you are in a horizontal position, gravity no longer helps prevent stomach acid from flowing back into the oesophagus.
In addition, swallowing occurs less frequently during sleep, reducing the natural clearance of acid. As a result, acid may remain in the oesophagus for longer periods, leading to irritation and disrupted sleep.
Lifestyle measures that help manage GERD symptoms
In many individuals, simple lifestyle changes can help lessen the frequency and severity of reflux symptoms:
- Eat smaller, more frequent meals – avoid overeating or late-night suppers.
- Wait at least 2–3 hours after eating before lying down or going to bed (Or plan your dinners earlier)
- Elevate the head of your bed slightly to reduce nighttime reflux.
- Maintain a healthy weight to reduce pressure on your stomach.
- Avoid trigger foods such as caffeine, chocolate, onions, citrus, and spicy dishes.
- Quit smoking and limit alcohol.
- Wear looser clothing to reduce pressure on your abdomen
Can GERD improve on its own?
Mild reflux can improve with lifestyle changes, but chronic GERD rarely resolves without proper evaluation.
If not intervened in time, this frequent acid backwash can damage your oesophagus, leading to conditions like oesophagitis, strictures or Barrett’s oesophagus.
If you find yourself relying on medication more than twice a week, or if symptoms begin to affect your sleep, appetite, or voice, it may be time to consider consulting a gastroenterologist for further assessment.
Support and care for ongoing GERD symptoms

If you continue to experience heartburn, chest discomfort, or throat irritation despite lifestyle adjustments, further assessment may be helpful.
At Richmond Gastroenterology Centre, Dr John Hsiang provides careful evaluation of reflux symptoms, including gastroscopy where appropriate, to better understand the underlying cause and guide management.
If you have concerns about ongoing reflux symptoms, you may consider arranging a consultation for a personalised assessment and discussion of suitable care options.
References:
1. Kahrilas P. J. (2003). GERD pathogenesis, pathophysiology, and clinical manifestations. Cleveland Clinic journal of medicine, 70 Suppl 5, S4–S19. https://pubmed.ncbi.nlm.nih.gov/14705378/
In Singapore, GERD affects an estimated 1 in 5 people, and local studies have shown that reflux symptoms have risen significantly over the years, mirroring increasing rates of obesity and modern lifestyle habits across Asia.GERD affects up to 20% of people in Singapore
The content on this website, including text, graphics, images, and information, is meant for general informational purposes only and should not be used as a substitute for professional medical advice, diagnosis, or treatment. RICHMOND ENDOSCOPY AND GASTROINTESTINAL SPECIALISTS PTE. LTD takes no responsibility if the information on this website is used without consulting one of its specialists.


